Functional Testing in Valdosta, Georgia
Comprehensive Stool Testing
Adrenal and Reproductive Hormone Levels
Functional Thyroid Testing
How Labs Determine “Normal” Ranges
If you have the symptoms of low thyroid hormone but your TSH is “normal,” something is not being addressed. Part of the problem starts with the reference range for what is considered normal. How do we get the “normal” lab range? The reference range is based on a statistical average of the population getting tests out of the lab. This is why (other than for vitamin D and cholesterol levels) lab reference ranges will vary depending on the lab.
The people who get tested in labs – in other words, the population of that lab – are obviously statistically not the healthiest segment of the population. Otherwise, they wouldn’t be getting lab tests. That means if the lab results are “normal” despite your symptoms, what your doctor is essentially saying is you’re just like a lot of other sick people!
In functional medicine, we look at a much narrower range of normal, taking this into account. We want your labs to look like a bunch of healthy people whose bodies function optimally and who feel great.
CardioMetabolic Testing
Your cellular metabolism and your cardiovascular system (heart and blood vessels) are very intricately linked. For various reasons – not just age – our metabolism changes. Our personal chemistry controls these changes and they can be measured in the CardioMetabolic panel. This covers the three main areas of keeping a healthy metabolic profile for life: Glycemic Control, Lipid Profile, and Vascular Inflammation.
- Lipoprotein Fractionation
- Lipoprotein Particle Numbers
- Total LDL Particles
- Total HDL Particles
- Triglycerides
- Lipoprotein (a)
- Leptin
- Apolipoprotein B
- hs-CRP
- Homocysteine
- Insulin
- Glucose
- Hemoglobin A1c
- C-peptide
- Adiponectin
- OmegaCheck
Food Sensitivity Testing
Many people have hidden underlying food intolerances that they are not aware of. The more common ones are dairy products, eggs, and wheat, but some are unexpected and surprising, such as garlic, bananas and cranberries. Foods that may be seemingly “healthy” foods may not be healthy for a specific individual. One way to identify food sensitivities is by doing an elimination and challenge test, which involves following a very restricted diet for 21 days (no eggs, dairy, nuts, shellfish, citrus, gluten, soy etc.) then reintroducing one food at a time to see what triggers symptoms. The elimination diet is considered the "gold standard" for evaluating food allergies.
This is a long and tedious process which the patient must be willing to do.
However, doing a finger-stick test shortcuts this, and assesses for 96 different foods. These are not full-blown food allergies, which are mediated by IgE cells that may manifest as anaphylaxis, rashes, swelling etc. occurring immediately after the food is eaten. Those are typically known about already. What we are looking for are IgG reactions which are delayed (up to 72 hours after eating the food), subtle and may manifest in any way from general fatigue and malaise to skin break outs to headaches. Most people who do this test find it fascinating, and avoiding their food sensitivities has allowed them to get to a higher level of health.
Gluten Intolerance Testing
Gluten intolerance is so common in the western world, but is underrecognized. Gluten intolerance may be a precursor to Celiac disease, but will not necessarily progress to that level of severity. Certainly many people can be gluten intolerant without having the diagnosis of Celiac without having the severe intestinal symptoms (diarrhea, malabsorption, weight loss etc. ) we associate with Celiac. I have seen arthritic symptoms, skin rashes, chronic fatigue, neurological issues and hormone imbalance all resolve by identifying gluten intolerance and adopting a gluten-free diet.
Heavy Metal Testing
Heavy metals such as lead, mercury and aluminum are neurotoxins, and can impact neurological function profoundly. Given that so many disorders today have their basis in the central nervous system (MS, Parkinson's, Alzheimer's, autism) or impact the nervous system secondarily (Lyme disease is a great example), anything we can do to release toxins from that system will help significantly in overall health. Even in the absence of “disease”, heavy metals may impact memory, ability to focus and concentrate, and the some of the 5 senses such as hearing and vision. It has also been well documented that cadmium and lead toxicity can contribute to development of hypertension.
Urinary Hormone Metabolite Testing
Urine testing for comprehensive hormones is a urine steroid hormone profile that measures cortisol pattern (circadian rhythm) as well as steroid/sex hormones, including DHEA, testosterone and androgens, estrogens and progesterone and also includes melatonin.
This easy to collect test is taken from the comfort of your home gives you valuable insight into your hormone production as well as the function of the hormone metabolism pathways (metabolites).
This comprehensive test also details your ability to DETOXIFY by showing estrogen metabolism in the liver and through methylation. This can be a very important factor to consider in those wishing to start hormone replacement therapy with a family history of breast or prostate cancers.
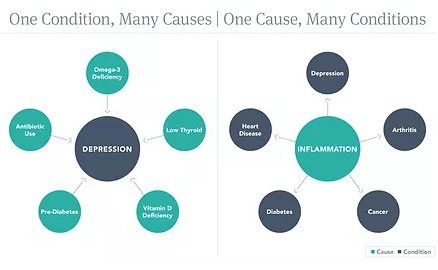
It can also show if there might be underlying INFLAMMATION and even if there is a possible thyroid imbalance.
This test can provide valuable information about the root causes of your symptoms.
Micronutrient Testing
Micronutrient testing provides the most comprehensive nutritional analysis available by measuring functional deficiencies at the cellular level. It is an assessment of how well the body utilizes 33 vitamins, minerals, amino/fatty acids, antioxidants, and metabolites, while conveying the body’s need for these micronutrients that enable the body to produce enzymes, hormones, and other substances essential for proper growth, development, and good health.
This test provides the basis of a personalized, functional approach in addressing a broad variety of clinical conditions including arthritis, cancer, cardiovascular risk, diabetes, various immunological disorders, metabolic disorders and micronutrient deficiencies.
Lyme Western Blot Test
Lyme is prevalent everywhere, and has far-reaching effects on the body. It can resemble chronic fatigue syndrome, fibromyalgia, MS, arthritis, Parkinson's, ALS and a host of others chronic illnesses. It is sneaky, and is spreading throughout the world – currently it is recognized as the fastest-growing infectious disease in the United States. However other infections can be introduced with the same exposure such as Bartonella, Babesia, mycoplasma, Ehrlichia, & RMSF.
There is also an association between Lyme disease and autism. One of the problems to date is that lab testing is unreliable, and this continues to be a challenge. There are several more sensitive lab testing options available aside from the standard western blot which can produces any false negatives in those with chronic disease and depressed immune function. If you are interested in taking a look at a very good online resource ILADS.org is a good place to start.
Genetic Testing
Upon completion of the mapping of the human genome, we know there are 20-25,000 genes in each genome. With this knowledge came the information that there are over 80 million variants in the human genome.
These variants are comprised in part of single nucleotide polymorphisms (SNPs) and deletions or insertions in the genome. It is these SNPs that provide significant health information to providers of integrative and functional medicine to prevent or alleviate chronic illness conditions.
Knowing the presence of and placement of SNPs through genetic point mutation testing allows evaluation of the susceptibility to develop many of the chronic illness conditions that affect people today. In addition, this kind of testing helps pinpoint relevant SNPs and their corresponding metabolic markers in individuals.
Testing of this kind provides targeted interventions through the use of traditional medicine approaches as well as supplementation through integrative and functional medicine approaches. Monitoring of individuals’ progress is also made easier with genetic testing by measuring metabolic markers found in the original tests over a period of time.
Individual monitoring of this type is necessary when this kind of personalized intervention and supplementation is used. If there is an overload of either medications or supplementations, there can be an impact on the performance of metabolic processes that can lead to side effects. These side effects can influence functions and responses, such as the immune response.
Individual SNPs will determine how well medications and supplements
COMT and CYP19 Genes and Weight Loss
Research has identified certain genes that work together and appear to show that some people retain fat regardless of, or in spite of, exercise.
In one study, researchers found two genes, COMT and CYP19 that appeared to be involved in patterns of fat loss and exercise. Having one CYP19 gene and variants of that gene did not affect fat, intra-abdominal fat, or total fat. However, having two of these genes seemed to be related to a slight decrease in body mass index and significantly more decrease in total fat and percentage of body fat.
The researchers also found that having one genotype of the COMT gene and one copy of the CYP19 gene seemed related to significant loss of BMI, total fat, and percentage of body fat.
Why and how these genes and combinations work isn’t known yet. More research is needed to determine this. Other research suggests women with a specific CYP19 variant may also have increased levels of estradiol and estrone which may make it harder for them to lose fat through exercise.
Analyzing Genetic Results
Variants in SHBG, DHFR, COMT, and CYP1B1.
SHBG: Sex Hormone Binding Globulin (SHBG) is synthesized in the liver, and in the blood, it transports and regulates the access of sex steroids to sex hormone receptors throughout your body. Research has found that isolated fructose has the most negative effect on SHBG levels, while also being connected to cancer growth by enhancing protein synthesis and promoting a more aggressive cancer phenotype.
The results for the SHBG gene variants have different nutrigenomic solutions based on whether your patient is male or female. For women, if estrogen is high and progesterone is low, these patients require a higher fiber intake, magnesium, vitamin A, C, E, B6, selenium, and L-arginine.
For men, if testosterone is low (variants in SHBG rs6258), increased magnesium, zinc, vitamin D, omega-3’s, boron and a higher healthy fat intake (if testosterone is low and depending on the fat genes) may be required along with weight lifting.
DHFR: Folic acid from fortified grains and supplementation slows down the DHFR gene and potentially blocks folate receptors, increasing cancer risk.
COMT: Oral contraceptives deplete folate, vitamins B2, B6, B12, vitamin C and E, magnesium, selenium, and zinc while slowing down COMT. Stress and the catechols from the coffee or green tea and red wine slow COMT further, causing disrupted sleep and increased anxiety/stress hormones. One study found K-Ras gene mutations – common in many cancers – were 4 times higher in coffee drinkers due to the chemical load of the organochlorines (non-organic coffee beans are one of the highest sprayed crops). The wine compounds the chemical load. A poor diet and magnesium deficiency has lead to struggles with disrupted gut flora and constipation, clogging up her liver with genotoxic estrogen.
CYP1B1: A higher activation rate of catechol estrogens may be occurring, causing more DNA damage and cancer risk.
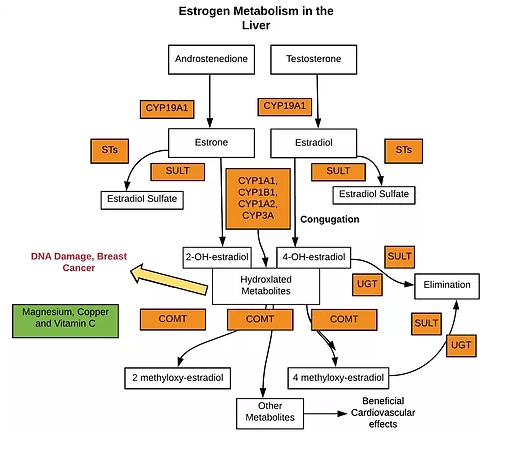
Cytochrome P-450 SNPs and Estrogen Detoxification
The major oxidative routes of estrone and estradiol are 2- and 4-hydroxylation by cytochrome P450 CYP1A1, CYP1B1, CYP1A2 and CYP3A. CYP1A1, CYP1B1 and CYP1A2 are in the detoxification section. CYP1A2 is also in the cardiovascular section for caffeine metabolism.
CYP1A1: CYP1A1 is also involved in the metabolism of benzopyrene (a polycyclic aromatic hydrocarbon) which disrupts DNA methylation and affects breast cancer growth. Variants in CYP1A1*2C is connected to lung health in Chinese, and breast and prostate health in Caucasians.
CYP1B1: The CYP1B1 polymorphism is an ultra-rapid metabolizer, and metabolizes procarcinogens such as polycyclic aromatic hydrocarbons and 17 beta-estradiol. This means that variants cause this enzyme to move too fast, creating carcinogenic activation of polycystic aromatic hydrocarbons and estrogens to genotoxic catechol estrogens – both which cause DNA mutations – with implications for breast, ovarian, colon, lung and prostate health. Inhibiting this liver enzyme with the flavonols quercetin, apigenin and myricetin helps lower the carcinogenic activity.
CYP1A2: A homozygous CYP1A2 is also a rapid metabolizer, metabolizing various environmental procarcinogens, such as heterocyclic amines, nitrosamines, aflatoxin B1 and ochratoxin A. As many of you know, aflatoxin is one of the most carcinogenic compounds known and is found in poorly stored peanuts, Brazil nuts, corn and grain-fed dairy. Ochratoxin A is a potential human carcinogen and may cause neurotoxic damage, immunosuppressive effects, and reproductive harm. 70% of oat-based cereals purchased in the U.S. were contaminated with the fungal toxin ochratoxin A. Wheat (32%) was the second highest in contamination with corn and rice having 15% each. The highest DNA toxicity of ochratoxin A in a study was found in cells where CYP1A2 was expressed.